New Advances in Testicular Cancer Awareness, Diagnosis, and Treatment as Global Health Efforts Intensify
Introduction
Testicular cancer has become one of the most discussed health topics among men’s health experts due to its rising awareness campaigns, improved screening technologies, and growing public understanding of early symptoms. Although it remains a relatively rare disease, testicular cancer predominantly affects younger men, typically between ages 15 and 40, making education and timely intervention essential. The growing attention from healthcare organizations and researchers worldwide has significantly improved survival rates and treatment pathways.
As medical advancements expand across cancer research and urology, global organizations are investing in better diagnostic systems, personalized treatment strategies, and long-term recovery support. This comprehensive article explores the evolution of testicular cancer management, from early detection to survivorship, offering readers an in-depth understanding of how this condition is approached today.

Understanding Testicular Cancer in Modern Healthcare
Testicular cancer is a malignancy that develops in the testicles, the organs responsible for producing sperm and hormones like testosterone. Although it represents a small percentage of all male cancers, it is the most common cancer in younger adult males. Increased awareness and education have contributed to earlier detection and better treatment outcomes.
Many men first notice symptoms such as swelling, lumps, or discomfort in one testicle. Because testicular cancer often presents with mild or painless signs, individuals may delay seeking medical attention. Healthcare providers emphasize the importance of regular self-examinations and awareness of risk factors to promote early diagnosis.
Key Characteristics of Testicular Cancer
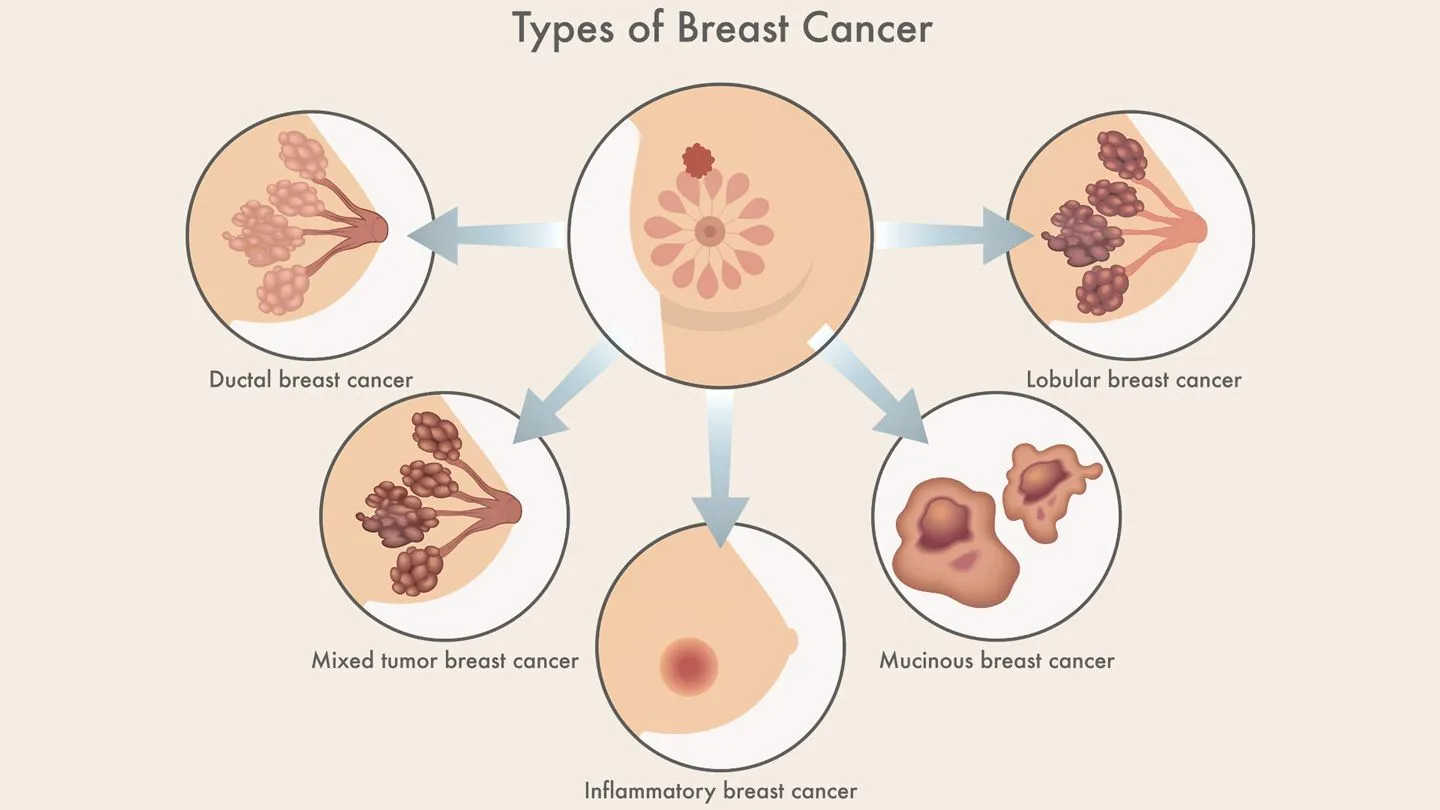
Testicular cancer primarily includes two main types: seminomas and non-seminomas. Each grows differently and responds to treatment uniquely. Understanding these differences helps guide treatment planning and patient support.
Risk Factors
- Family or personal history
- Undescended testicle (cryptorchidism)
- Certain genetic conditions
- Age patterns affecting young adults
The Importance of Early Detection and Diagnosis
Early detection greatly improves survival rates, as testicular cancer is highly treatable at early stages. Modern diagnostic technologies and public health campaigns encourage proactive self-checks and timely medical evaluations.
Diagnosis often includes a combination of physical examinations, ultrasound imaging, and blood tests that detect tumor markers. When caught early, treatment is often less invasive and more effective, improving quality of life for patients.
Common Diagnostic Tests
Ultrasound scans remain the gold standard for identifying abnormalities in testicular tissue, while tumor markers such as AFP, hCG, and LDH provide critical information about cancer type and progression.
Benefits of Early Detection
- Higher cure rates
- Less aggressive treatment required
- Shorter recovery times
Testicular Cancer Staging and What It Means for Treatment
Once diagnosed, doctors classify testicular cancer into stages based on how far it has spread. Staging is essential because it determines the most appropriate treatment plan and helps predict recovery outcomes.
Stage I cancer is confined to the testicle, while Stage II and III indicate spread to lymph nodes or distant organs. Understanding staging empowers patients and families to make informed decisions.
How Staging Works
Staging includes tumor size, lymph node involvement, and presence of metastasis. These factors together create a roadmap for treatment teams.
Patient Considerations
- Treatment intensity differs with stage
- Follow-up care becomes more extensive at later stages
Modern Treatment Methods for Testicular Cancer
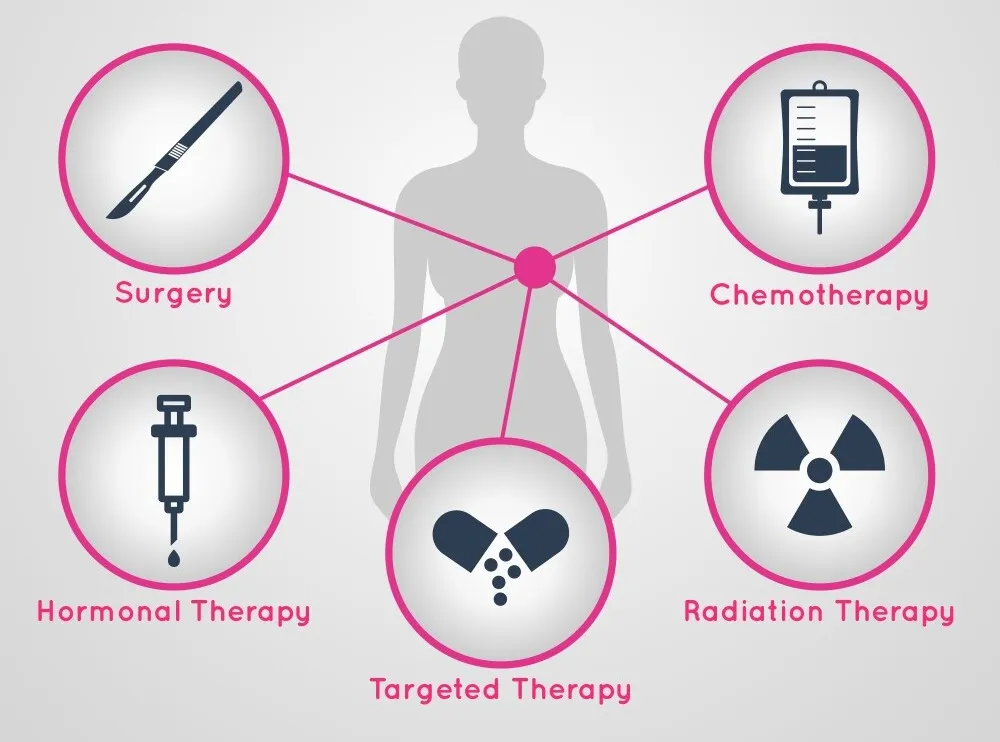
Treatment options for testicular cancer have evolved significantly, combining surgical approaches, radiation therapy, and chemotherapy depending on cancer type and stage. Today’s treatment plans emphasize both effectiveness and preservation of future fertility.
Most patients begin with surgical removal of the affected testicle (orchiectomy). This procedure is highly successful and forms the foundation of treatment for nearly all cases.
Common Treatment Options
- Surgery
- Radiation (primarily for seminomas)
- Chemotherapy for advanced or aggressive cancers
Treatment Goals
- Remove cancer
- Prevent recurrence
- Maintain long-term health and fertility
Surgical Approaches and Recovery
Surgery remains the frontline treatment for testicular cancer, offering high cure rates when the disease is detected early. Most procedures involve removing the cancerous testicle through a minimally invasive incision.
Recovery times are relatively short, with most patients resuming daily activities within a few weeks. Surgeons also consider cosmetic and psychological factors, offering testicular implants for those who prefer them.
Post-Surgery Care
Patients often undergo monitoring through blood tests and imaging to ensure cancer does not return.
Benefits of Surgical Treatment
- Immediate removal of cancer
- Minimal long-term physical limitation
Chemotherapy and Radiation in Testicular Cancer Care
Chemotherapy plays a vital role in treating advanced testicular cancer, especially cases involving metastasis or aggressive cell types. Drug combinations such as BEP (Bleomycin, Etoposide, Cisplatin) are widely used.
Radiation therapy, while less common today, remains effective for certain seminomas due to their high sensitivity to radiation. Both methods have contributed to significantly improved survival rates.
Managing Side Effects
Doctors help patients manage temporary side effects such as fatigue, immune suppression, or nausea through supportive medications.
Why These Treatments Work
Chemotherapy and radiation target fast-growing cancer cells while sparing most healthy tissue.
Fertility Preservation and Emotional Support
Because testicular cancer often affects individuals in their reproductive years, fertility preservation is a key part of treatment planning. Many healthcare providers recommend sperm banking before treatment begins.
Beyond physical health, emotional well-being is equally important. Counseling, support groups, and survivorship programs provide encouragement and guidance throughout the treatment journey.
Fertility Options
- Sperm banking
- Hormonal evaluations
- Post-treatment reproductive counseling
Psychological Support
- Therapy
- Peer support networks
Life After Treatment and Long-Term Survivorship
Survivorship for testicular cancer patients is typically positive, with many individuals returning to normal life following treatment. Long-term checkups, including blood tests and scans, help ensure continued health and detect any potential recurrence early.
Many survivors report improved outlooks on life and health, engaging more actively in wellness habits such as exercise, balanced nutrition, and stress management.
Follow-Up Recommendations
Regular medical visits often continue for several years, depending on treatment type and cancer stage.
Survivorship Challenges
- Adjusting physically and emotionally
- Monitoring long-term treatment effects
Innovations and Future Trends in Testicular Cancer Research
Research in testicular cancer continues to evolve, focusing on more precise diagnostic tools, minimal-toxic treatment methods, and advanced genetic testing. Scientists aim to personalize treatment even further to reduce side effects and improve cure rates.
Immunotherapy, targeted molecular drugs, and improved imaging systems are among the most promising developments expected to influence future care.
Emerging Research Areas
- Genetic profiling
- Immunotherapy advancements
- Improved surgical technologies
Long-Term Impact
These innovations hold the potential to eliminate recurrence and minimize treatment complications for future generations.
Global Awareness Efforts and Public Education
Global health organizations, advocacy groups, and nonprofit foundations continue expanding educational campaigns to increase awareness of testicular cancer. These initiatives promote routine self-checks, early diagnosis, and open conversations about men’s health.
Public campaigns during Men’s Health Month and other awareness events have significantly reduced stigma, encouraging men to seek medical advice promptly when symptoms appear.
Key Awareness Strategies
- Community outreach
- Digital education tools
- Partnering with sports and media organizations
Why Awareness Matters
Early action remains the strongest factor in improving testicular cancer outcomes.
Conclusion
Testicular cancer has become one of the most successfully treatable cancers thanks to early detection, modern surgical techniques, advanced therapies, and growing public awareness. The continuous development of new diagnostic tools, research innovations, and global educational campaigns is making testicular cancer treatment more effective and accessible than ever before. With improved survivorship programs and strong healthcare support systems, patients today can look forward to healthier, empowered futures. As awareness continues to rise, early recognition and timely treatment will remain essential in reducing the burden of this disease worldwide.